The AI-native analytics platform that turns claims intelligence into closed care gaps, improved Star Ratings, and measurable ROI — at a fraction of legacy cost.
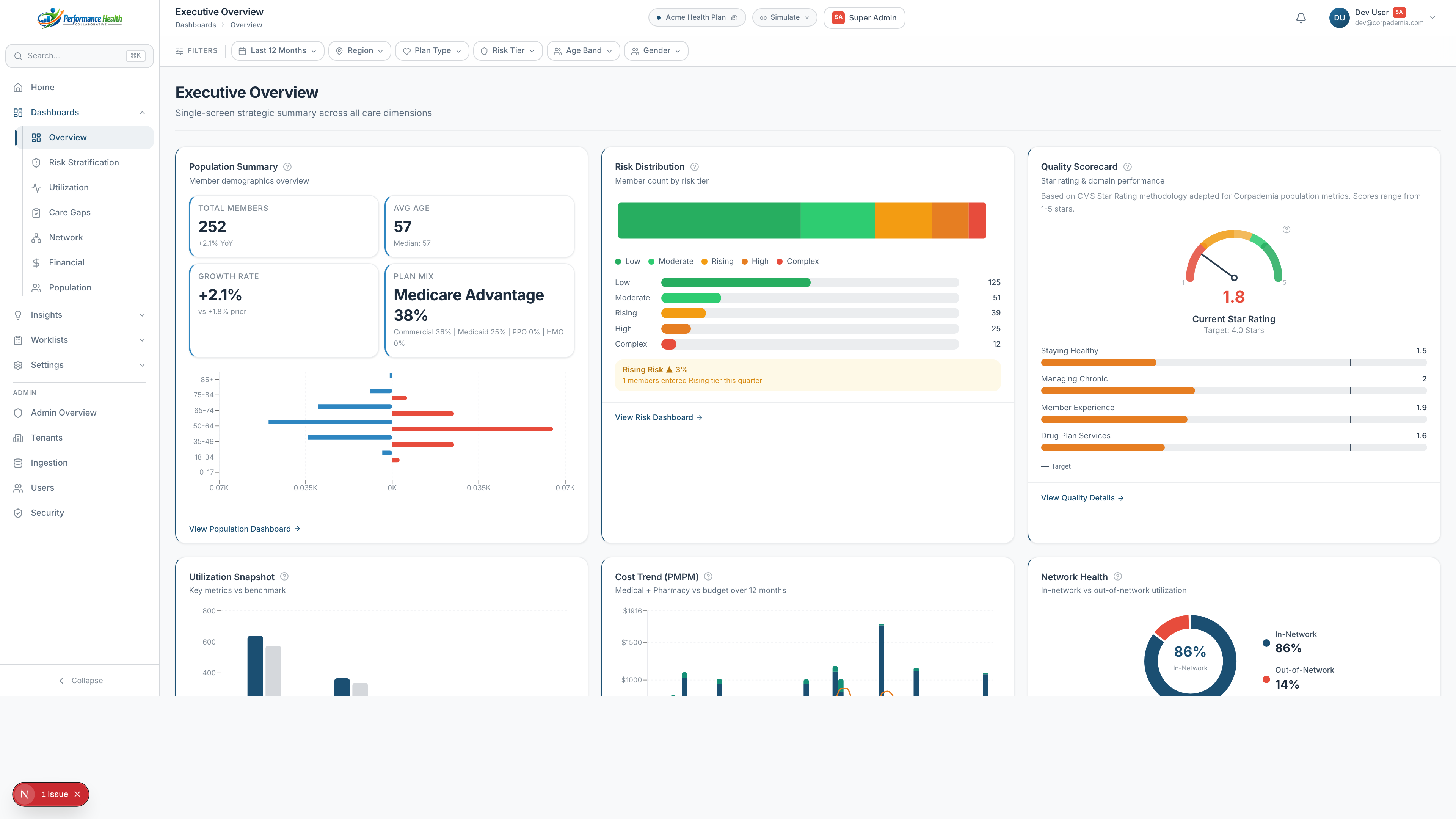
Legacy analytics stacks report on the past. Your members need action today.
Purpose-built analytics for every stakeholder — from the CMO to the care manager — all drawing from a single source of truth.
KPI command center with AI-generated narrative insights across all domains.
CMO · VP Quality5-tier risk model with rising-risk intervention triggers and cost predictions.
Care ManagementED, inpatient, readmission trends with network leakage detection.
Utilization Review32 HEDIS measures with AI-enriched gap closure recommendations.
Quality · HEDIS TeamsProvider scorecards, referral patterns, and panel capacity analysis.
Network ManagementPMPM trends, medical loss ratio tracking, and cost-of-care cohort analysis.
CFO · ActuarialDemographic segmentation, social determinants, chronic disease prevalence.
Population Health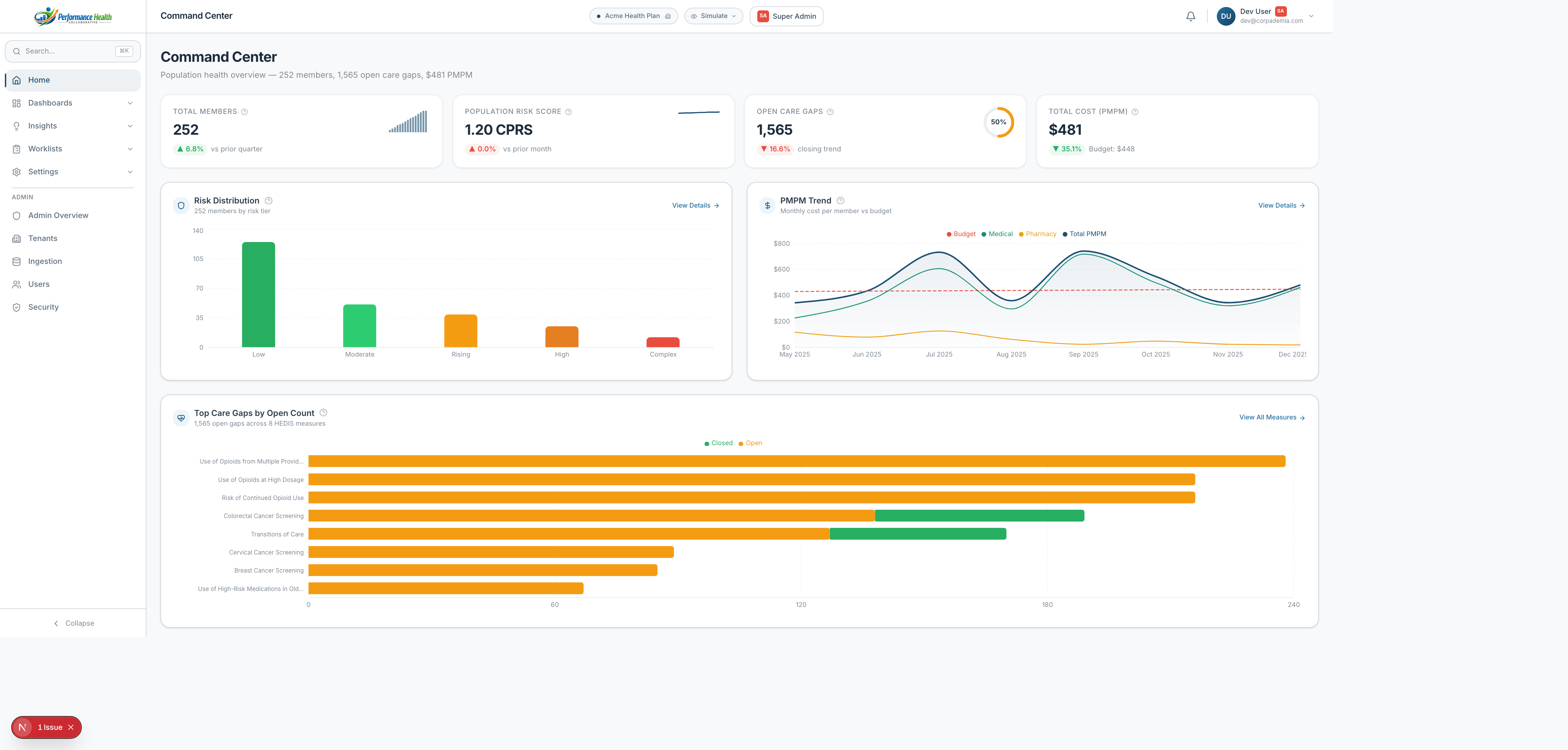
Every feature is designed to move from insight to intervention — automatically.
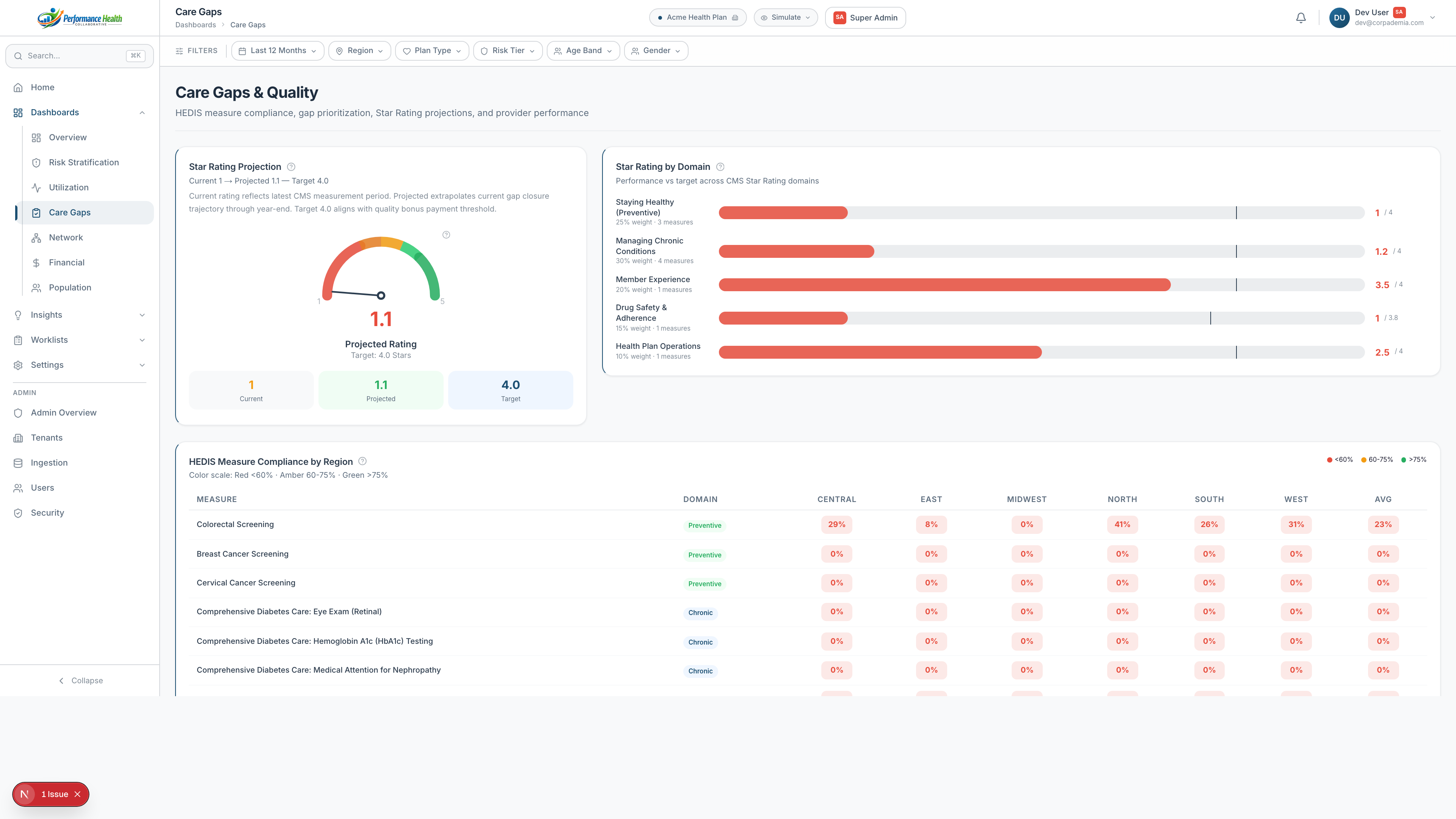
Our care gap detection engine implements 32 HEDIS MY2024 measures across 7 clinical domains — not as probabilistic guesses, but as deterministic SQL logic running against your claims data.
Our AI insights engine analyzes your entire population nightly and surfaces what’s changed, what’s at risk, and what to do about it. Then ask any question in plain English.
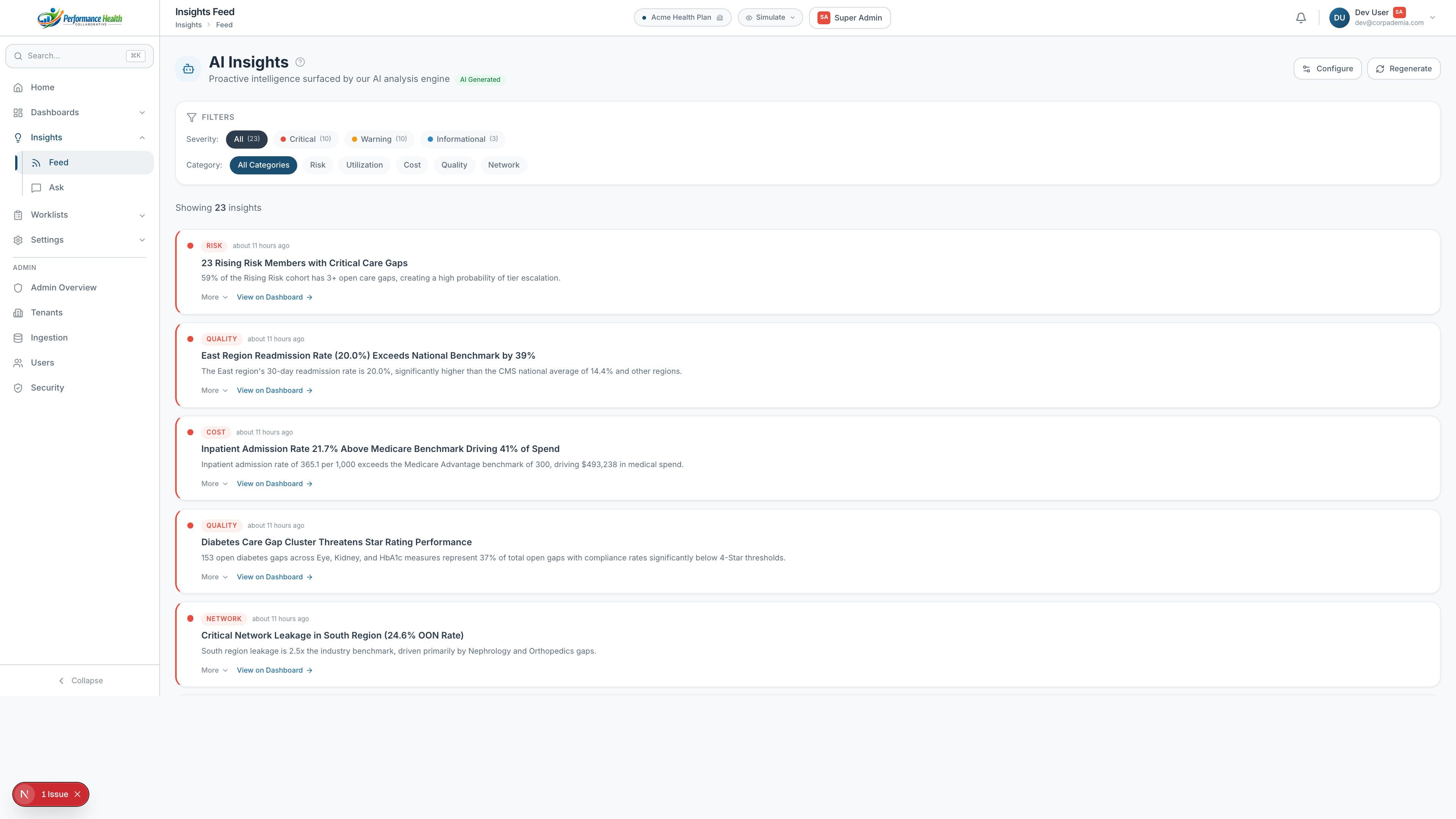
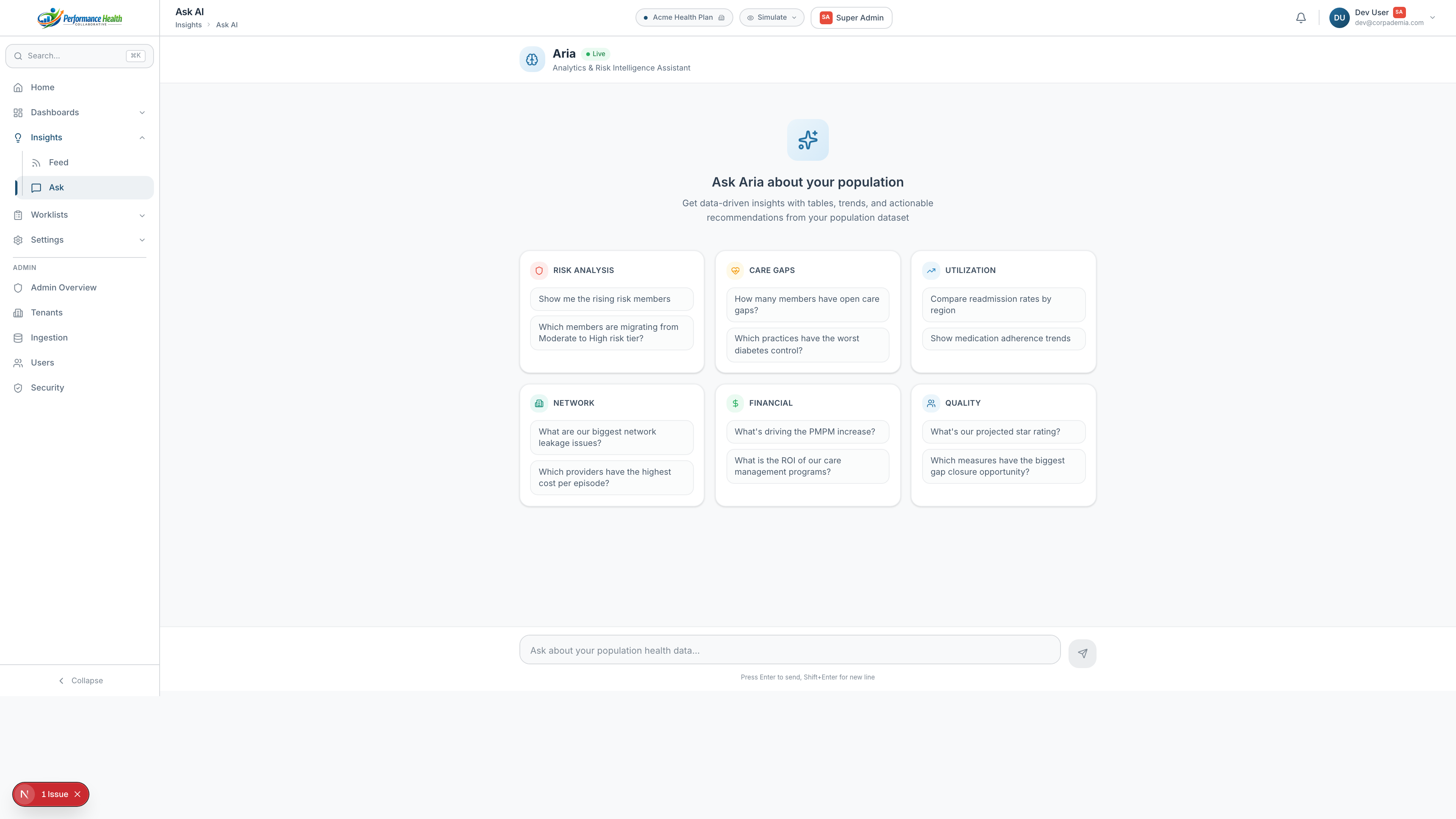
Our 5-tier risk model identifies members who are becoming expensive — not just those who already are. When a member enters the Rising tier, outreach triggers automatically.
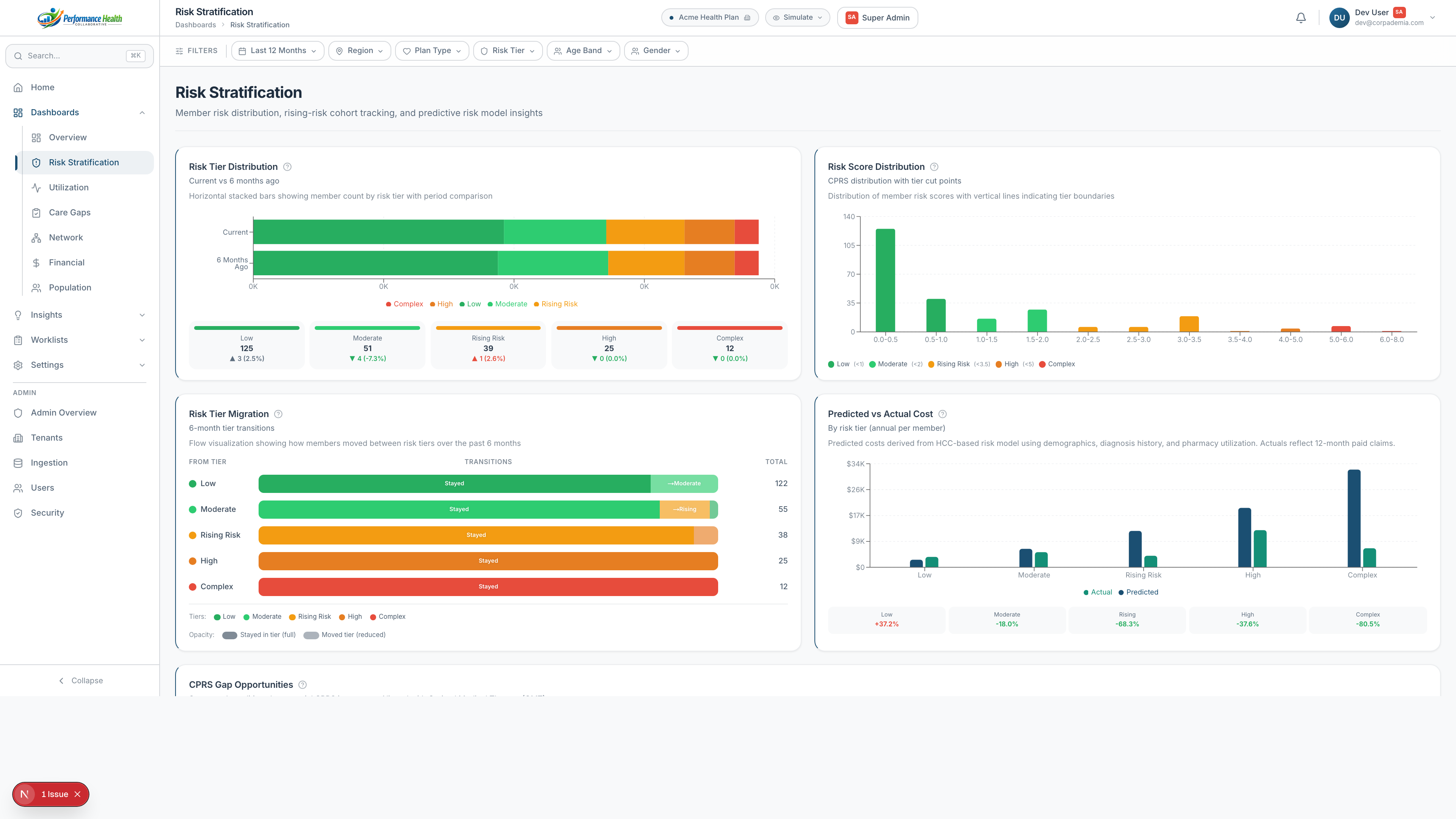
From gap detection to closed loop — fully automated. AI generates personalized outreach per member, per gap, across email, SMS, and AI voice with automated follow-up sequences.
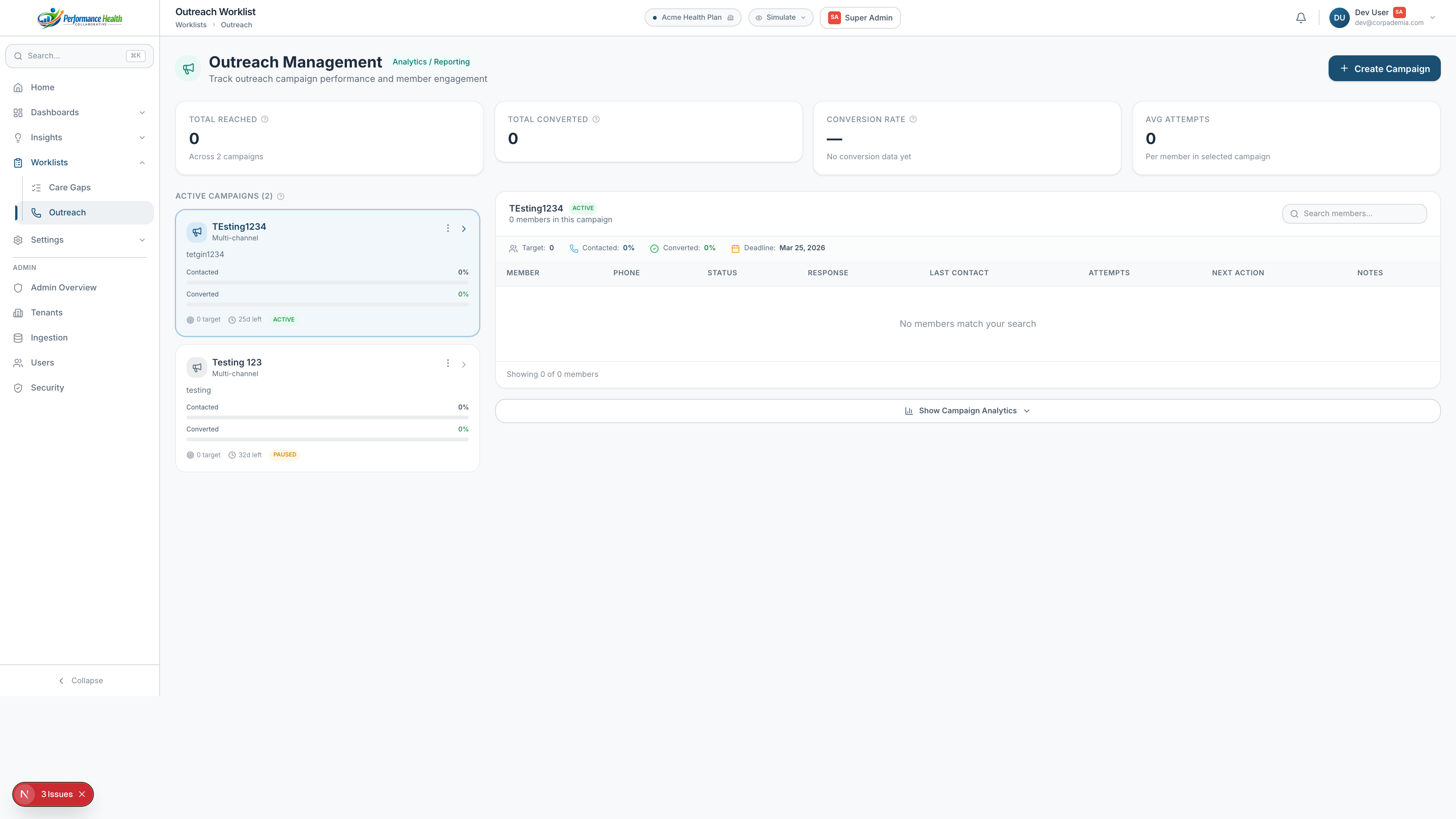
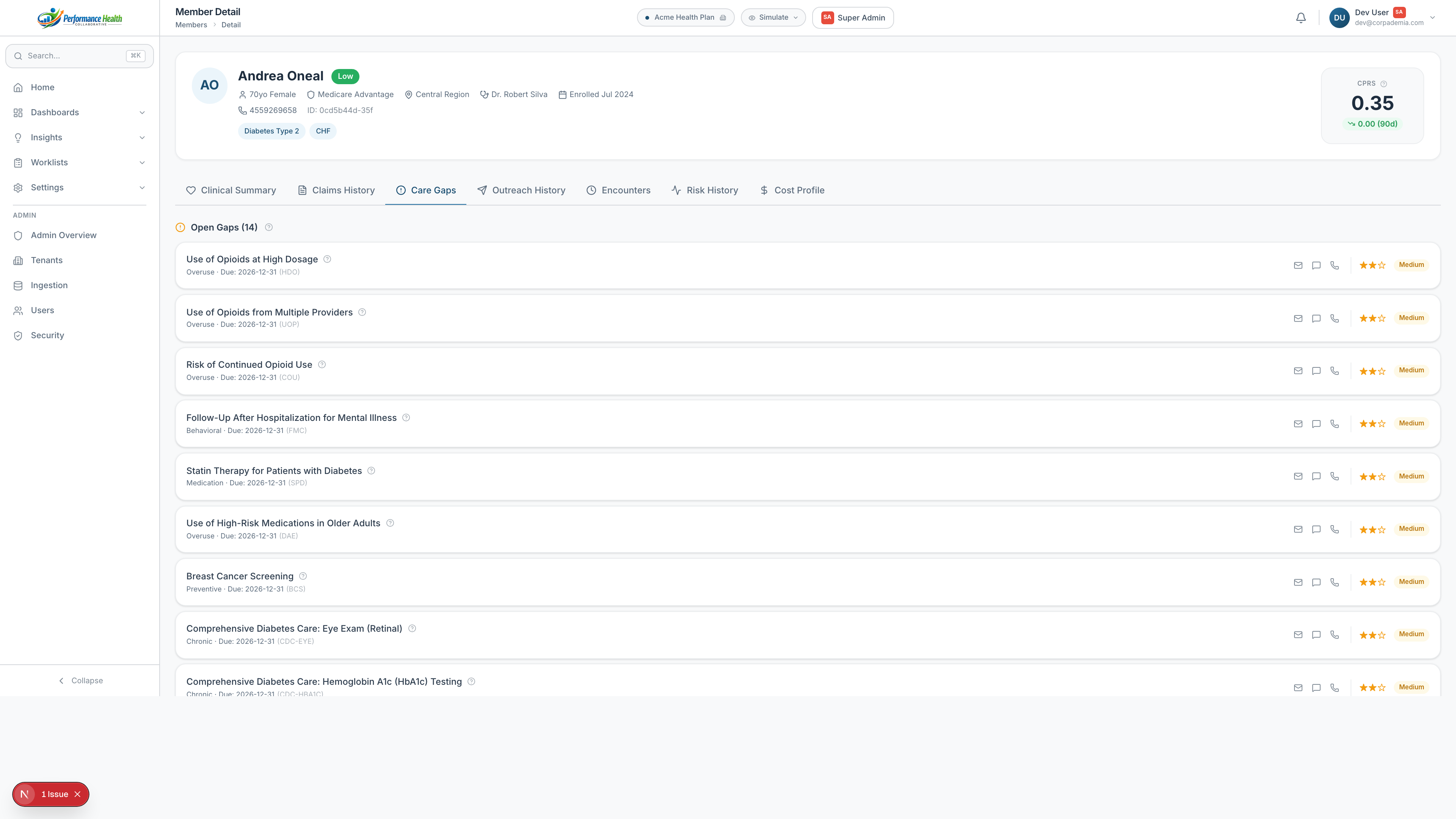
Built into every layer — not bolted on after the fact.
Transparent PMPM pricing. No hidden fees. No long-term lock-in.
| Legacy Stack | HealthBenIQ | |
|---|---|---|
| PMPM Cost | $8 – $15 | $1.00 – $1.50 |
| Implementation | 6 – 12 months | 6 weeks |
| Action Layer | None | AI Outreach Built-In |
| Annual Cost (100K members) | $9.6M – $18M | $1.2M – $1.8M |
| Savings | 85–90% reduction |
Three scenarios that demonstrate why the platform pays for itself in weeks, not years.
No professional services fees. No consultants. No 12-month project plan.
See your data in the platform — not a canned demo. We’ll load a sample of your claims and show real insights in 30 minutes.